
Surgical procedures for fertility issues sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail with casual formal language style and brimming with originality from the outset.
As we delve into the complexities of surgical procedures aimed at addressing fertility concerns, a world of possibilities unfolds, shedding light on the intricate solutions available for individuals seeking to enhance their reproductive health.
Surgical Procedures for Fertility Issues
When other fertility treatments have not been successful, surgical procedures can be considered to address underlying issues that may be affecting a couple’s ability to conceive. These procedures aim to correct anatomical abnormalities, remove blockages, or improve reproductive function.
Types of Surgical Procedures
- Laparoscopic Surgery: A minimally invasive procedure performed through small incisions in the abdomen to treat conditions such as endometriosis, ovarian cysts, or blocked fallopian tubes.
- Hysteroscopic Surgery: Used to correct issues within the uterus, such as polyps, fibroids, or septum, which may be impacting fertility.
- Tubal Reanastomosis: A procedure to reconnect the fallopian tubes after a previous tubal ligation, allowing for natural conception.
Common Fertility Issues Requiring Surgery
- Endometriosis: A condition where tissue similar to the lining of the uterus grows outside the uterus, causing inflammation and scarring.
- Fibroids: Noncancerous growths in the uterus that can interfere with implantation or block the fallopian tubes.
- Tubal Blockages: Obstructions in the fallopian tubes can prevent the egg from meeting the sperm, leading to infertility.
Benefits and Risks of Surgical Procedures
Surgical procedures for fertility issues can offer the benefit of correcting underlying problems that may be hindering conception, increasing the chances of natural pregnancy. However, these procedures also come with risks such as infection, bleeding, or damage to surrounding tissues. It is essential to discuss the potential benefits and risks with a healthcare provider before undergoing any surgical intervention.
Laparoscopic Surgery for Fertility
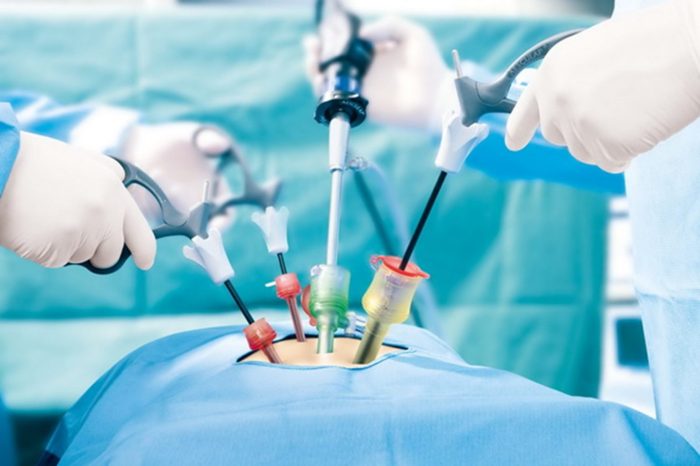
Laparoscopic surgery is a minimally invasive surgical procedure used to diagnose and treat fertility issues in both men and women. This technique involves making small incisions in the abdomen through which a laparoscope, a thin tube with a camera and light, is inserted to visualize the reproductive organs.
Comparison with Other Surgical Techniques
Compared to traditional open surgeries, laparoscopic surgery offers several advantages for treating fertility problems. It involves less scarring, reduced pain, shorter hospital stays, and faster recovery times. Additionally, laparoscopic surgery provides better visualization of the reproductive organs, allowing for more precise and targeted treatment.
Success Rates and Recovery Times
- Laparoscopic surgery has been shown to have high success rates in treating conditions such as endometriosis, ovarian cysts, and fallopian tube blockages, which can impact fertility.
- Recovery times after laparoscopic surgery are typically shorter compared to traditional open surgeries, with most patients able to resume normal activities within a few days to a week.
- Success rates and recovery times may vary depending on the specific fertility issue being addressed and the individual’s overall health.
Hysteroscopy for Fertility

Hysteroscopy is a minimally invasive surgical procedure used to diagnose and treat various fertility issues in women. By inserting a thin, lighted tube called a hysteroscope through the vagina and cervix into the uterus, doctors can examine the uterine cavity for abnormalities that may be affecting fertility.
Conditions Addressed through Hysteroscopy
- Uterine Polyps: Hysteroscopy can help identify and remove uterine polyps, which are growths in the lining of the uterus that can interfere with implantation of a fertilized egg.
- Uterine Fibroids: This procedure can also address uterine fibroids, noncancerous growths in the uterus that can impact fertility by distorting the uterine cavity or blocking the fallopian tubes.
- Uterine Septum: Hysteroscopy is used to correct a uterine septum, a band of tissue that divides the uterine cavity and can lead to recurrent miscarriages or infertility.
Role of Hysteroscopy in Improving Fertility Outcomes
- Diagnostic Tool: Hysteroscopy allows for a detailed examination of the uterine cavity, helping to identify and address any structural abnormalities that may be hindering fertility.
- Treatment: By removing polyps, fibroids, or correcting a uterine septum, hysteroscopy can improve the chances of successful implantation of an embryo and reduce the risk of miscarriage.
- Enhanced Success of Assisted Reproductive Techniques: Hysteroscopy can optimize the uterine environment for procedures like in vitro fertilization (IVF) by ensuring a healthy and receptive uterine lining.
In Vitro Fertilization (IVF) and Surgical Procedures
When it comes to addressing fertility issues, the combination of surgical procedures with In Vitro Fertilization (IVF) can significantly impact the success rates of fertility treatments.
Complementing Tubal Surgeries with IVF Treatment
Surgical procedures such as tubal surgeries play a crucial role in complementing IVF treatment. By repairing damaged or blocked fallopian tubes through surgery, IVF success rates can be greatly enhanced. When the fallopian tubes are functioning properly, the chances of successful embryo implantation and pregnancy through IVF significantly increase.
Significance of Pre-IVF Surgical Interventions
Pre-IVF surgical interventions are essential in preparing the reproductive organs for the IVF procedure. By addressing any underlying issues such as fibroids, polyps, or endometriosis through surgeries like hysteroscopy or laparoscopy before proceeding with IVF, the quality of the uterine environment is improved. This optimized environment can lead to better embryo implantation and overall success rates of IVF.
Coordination between Surgical Procedures and IVF
The coordination between surgical procedures and IVF is crucial for achieving better fertility outcomes. By strategically planning and timing surgical interventions before initiating IVF treatment, the reproductive system is primed for successful embryo transfer and implantation. This synchronized approach ensures that both the structural integrity of the reproductive organs and the hormonal balance necessary for IVF success are optimized, leading to improved chances of conception and a healthy pregnancy.
In conclusion, the realm of surgical procedures for fertility issues unveils a realm of hope and innovation, providing individuals with the opportunity to navigate their fertility journey with confidence and insight, ultimately leading to empowered reproductive well-being.
Detailed FAQs
What are the common risks associated with surgical procedures for fertility issues?
Common risks include infection, bleeding, and damage to surrounding organs, but these are usually rare and managed by skilled medical professionals.
How long does recovery typically take after laparoscopic surgery for fertility concerns?
Recovery times vary, but most individuals can resume normal activities within a week or two after laparoscopic surgery.
Can hysteroscopy help diagnose conditions that may be affecting fertility?
Yes, hysteroscopy is a valuable tool for identifying issues such as polyps, fibroids, or scar tissue that could be impacting fertility.





